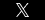The sinuses are vital aeration, drainage, and lubrication channels that keep the skull clear and the nasal passages free of invaders such as dust and pollen. The fine hairs that line the sinuses, known as cilia, act as a conduit for mucus drainage from the sinuses to the nose. Because the sinuses must remain clear for proper breathing, surgery is sometimes required to clear them when they become blocked due to growths, infections, or structural abnormalities. Call our office right away if you or a family member has been injured as a result of surgical malpractice. Our highly experienced medical malpractice attorneys at DeFrancisco & Falgiatano may be able to assist you in obtaining the compensation you deserve. We serve clients throughout Upstate New York and have offices in several convenient locations. Our extensive experience in the field of medical malpractice is reflected in the results we have obtained for our clients.
Individuals may undergo sinus surgery for a variety of reasons. If a person is born with bone deformities that block the sinuses or had trauma to the face that has left bones protruding into the sinuses, surgery may be required to remove sinus obstructions. Similarly, when tumors, polyps, or other nasal growths appear, they must be surgically removed or risk sinus blockages and infections that can cause swelling, which is another source of problems when they obstruct the free passage of mucus from the sinuses to the nose. Nasal polyps are small swellings in the nasal passages that can cause obstruction. They develop when the nasal lining becomes irritated and swollen, and they can cause breathing problems, face pain, runny nose, recurring infections, nasal congestion, and loss of smell.
Sinus infections or sinusitis may also necessitate surgery. Common sinusitis symptoms include a runny nose, congestion, headache, cough, pressure around the face, particularly around the eyes, nose, and brow, hearing loss due to ear blockage, and mucus dripping down the throat. When infections reoccur frequently, surgery to clear the passages and prevent future infections may be required. Most doctors will first try antibiotics before removing nodules or other obstructions surgically. To combat recurring infections, they may also recommend nasal sprays and rinses, steroids, allergy medications, and antihistamines. If everything else fails, surgery may be the only option.
Chronic sinusitis and related conditions are major medical problems in the United States and around the world, affecting more than 30 million Americans each year at a cost of more than 4.3 billion dollars. Over-the-counter and prescription medications account for the majority of the costs while providing little curative benefit in most chronic sinusitis patients. Surgical treatment of sinus disease is becoming more common, with an estimated 800,000 cases per year in the United States.
Historically, most sinus surgery was performed to treat the acute complications of a sinus infection. With modern medical care, these complications are far less common. In the United States, the majority of sinus-related surgical cases are currently functional endoscopic sinus surgery (FESS) for the treatment of chronic sinusitis. Any nasal procedure carries risks, such as nosebleeds, fainting, pain, and a rapid heartbeat after local anesthesia. A sinus puncture under your lip may also cause numbness in your cheeks or lips. Balloon sinuplasty is less invasive and has a lower complication rate than traditional sinus surgery.
Risks of balloon sinuplasty include mucosal/tissue damage from optic nerve expansion, which is uncommon, and infection. Complications from balloon sinuplasty are uncommon. It is best to have the procedure done by an experienced ENT surgeon. Make an appointment for a full consultation ahead of time so you know what to expect from the procedure and understand the benefits and risks for your specific situation.
Chronic disease is a more insidious group of illnesses that do not always manifest as a fungal or bacterial infection. Many cases are associated with other systemic diseases such as asthma, connective tissue disorder, uncontrolled allergic or inflammatory disease, or systemic immunologic dysfunction. When aggressive medical therapy fails to resolve functional obstruction of normal sinus opening by intranasal swelling, obstruction of the nasal passage itself by inflammatory diseases such as polyps, or recalcitrant sinus opacification, these procedures are performed.
Unfortunately, even with modern functional endoscopic techniques, sinus surgery leaves a lot to be desired for many patients. Unlike other general surgical procedures for infection prevention and treatment, such as appendectomy or cholecystectomy, sinus surgery for chronic sinusitis is frequently performed on a single patient multiple times and is rarely deemed curative.
The affected organ is not removed during sinus surgery; in fact, a poorly performed operation may make it more diseased. Many sinus patients are doomed to failure and recurrent surgery due to scar tissue formation, recurrence, the persistence of inflammatory or infectious conditions in the nose and sinuses, and untreated systemic illness.
Surgeons have become increasingly aware of the importance of preserving or restoring normal sinus anatomy. Modern FESS is based on the more anatomic and physiologic method of reopening and enlarging the natural drainage pathways from the sinuses to the nasal passages.
The FESS of today is vastly different from sinus surgery performed even a few years ago. Advanced rhinology and sinus surgery fellowship training provided by a dedicated rhinology faculty are becoming more common. Mucociliary clearance, the relationship between the sinus and pulmonary function, and the allergic and immunologic properties of the sinuses and nose have all advanced significantly in recent years.
Balloon sinus dilation (BSD) is the first step away from the destructive access techniques required for FESS and toward tissue preservation techniques. Similar to how an angioplasty is used to open coronary arteries and avoid bypass graft surgery, BSD allows patients with chronic sinusitis to preserve and restore their native sinus anatomy.
Balloon sinus dilation (BSD) treatment for sinus disease has the same indications as standard functional endoscopic sinus surgery (FESS). BSD, like FESS, is designed to provide as permanent access to and ventilation of obstructed sinuses as possible, allowing the normal function to resume and ongoing maintenance therapies to be effective.
While the vast majority of sinus surgeries are without complications, all surgeries carry inherent risks such as infection and bleeding. Patients may experience bleeding or a blood clot to the septum, the bone that separates the left and right nostrils, within a day of the procedure. The septum, as well as the eye, may be damaged during surgery if the bone between the eye and the sinus cavities is damaged. Bleeding into the eye can result in vision loss or distortion, such as double vision, as well as excessive tearing due to damaged tear ducts.
An infection may also develop if brain fluid spills into the surgical area. Meningitis, a potentially fatal brain infection, must be diagnosed and treated as soon as possible to avoid further complications. Complications can also include loss of taste, smell, or voice. Following surgery, the voice may also be altered. Although it is uncommon, scar tissue can cause the nasal airway passages to become partially blocked. While some potential complications are uncommon, infection and damage to adjacent bones and tissues to the surgical site are the most common causes of post-sinus surgery pain. Surgical-site infections, as well as infections affecting nearby organs or the brain, can be fatal.
Most patients go home within a day or two after surgery with gauze packed in their nose, which eventually dissolves or is removed by a doctor. Recovery time is relatively short, depending on the individual’s age and health. Pain medication and instructions on how to care for the surgical site to avoid infection are usually prescribed. When an infection occurs, antibiotics are usually prescribed to eliminate the infection as soon as possible. However, some patients discover surgical complications after leaving the hospital. Some even discover that the surgery did not resolve the issue for which they sought treatment, such as recurring infections or bone deformity obstructions. In some cases, surgeons made mistakes that resulted in worse health problems than the surgery itself, such as blindness, meningitis, or another serious complication.
Sinus surgery is typically performed by otolaryngologists, also known as ear, nose, and throat specialists. These doctors specialize in these diseases, so they are often the ones who diagnose and treat sinus problems, including recommending and performing surgery. Otolaryngologists are specialists in their field, which means they spend additional time learning about their specialty after medical school and interning in their specialty before practicing on their own. As a result, they should understand how to perform various sinus surgeries without endangering a patient who has entrusted them with ensuring a successful outcome.
Surgeons performing sinus surgery can make a variety of errors that could lead to medical malpractice litigation. For example, the surgeon may fracture one of your orbital bones, causing you to lose your sight indefinitely. During sinus surgery, your doctor may inadvertently cut the lowest of three bony structures on either side of the septum that functions as air warmers and airflow controllers. Other errors include operating on the wrong sinus site, which is sometimes caused by incorrect or misread radiological reports. Similarly, inadequate follow-up with patients who develop infections or continue to experience adverse symptoms as a result of improper surgical techniques or errors can have disastrous consequences. In all of these scenarios, sinus surgery doctors, hospitals, and their staff may be held liable for serious health consequences.
Sinus surgery is one of the more common surgeries, but patients are frequently harmed when doctors make errors that could have been avoided with proper attention, training, and medical practices. When a doctor performing sinus surgery injures you, you may be forced to have another surgery or surgeries to repair the damage. To live with the consequences of the damage, such as lost vision, you may require long-term or lifetime treatment. You should not have to pay for injuries caused by a medical professional’s negligent sinus surgery performance, and you may not have to.
Seek the help of an Upstate New York malpractice attorney on our team to explore your avenues of redress, such as monetary compensation for all the medical costs and lost wages incurred due to doctor visits, as well as for the pain and suffering you experienced due to unnecessary injury and long-lasting treatment. Medical mistakes can have deadly consequences. At DeFrancisco & Falgiatano, we represent injured clients and their families throughout Upstate New York, including Syracuse, Rochester, Albany, Buffalo, Elmira, Binghamton, Auburn, Ithaca, Oswego, Norwich, Herkimer, Delhi, Cooperstown, Cortland, Lowville, Oneida, Watertown, Utica, Canandaigua, Wampsville, Lyons, and surrounding areas. Please call us at 833-200-2000 or contact us via our online form to discuss your case.
 Rochester Medical Malpractice and Personal Injury Lawyer Blog
Rochester Medical Malpractice and Personal Injury Lawyer Blog